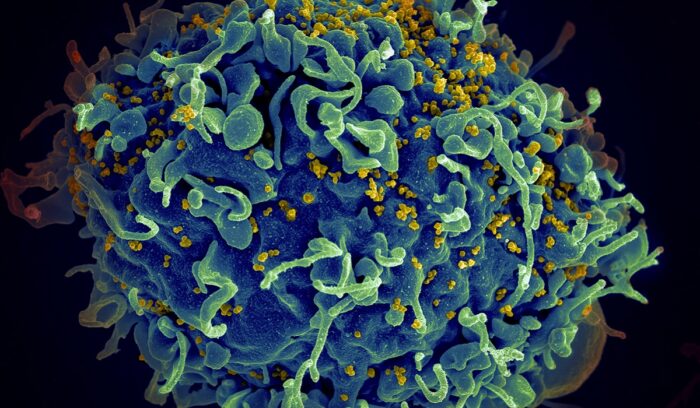
Zimbabwe made history by becoming the first country in Africa — and only the third in the world — to approve cabotegravir (CAB-LA), a long-acting injectable drug that significantly reduces HIV transmission. The World Health Organization called the move a “crucial step” and pledged to help Zimbabwe roll out programs to make CAB-LA as widely available and effective as possible.
At a glance
- CAB-LA approval: Zimbabwe joined Australia and the U.S. as the only countries to have approved the injectable drug, which the WHO recommended in July 2022 C.E. as highly effective at reducing HIV transmission among people at greatest risk.
- HIV prevention progress: AIDS-related deaths in Zimbabwe have fallen from an estimated 130,000 in 2002 C.E. to just 20,000 in 2021 C.E. — a reduction of more than 84% in less than two decades.
- 90-90-90 milestone: Zimbabwe already achieved the UNAIDS 90-90-90 target: 90% of people living with HIV know their status, 90% are on antiretroviral treatment, and 90% have the virus suppressed.
Why this drug matters
CAB-LA works differently from daily oral HIV prevention pills. Given as an injection every two months, it removes the burden of daily adherence — a major barrier for many people, particularly young women and girls in sub-Saharan Africa.
That matters enormously in Zimbabwe and across the region, where women and girls bear a disproportionate share of new HIV infections. Oral pre-exposure prophylaxis (PrEP) has existed for years, but daily pill regimens can be difficult to sustain in settings where stigma, privacy concerns, and inconsistent healthcare access all work against consistent use.
The WHO’s July 2022 C.E. recommendation described CAB-LA as highly effective for people at substantial risk of contracting HIV — a category that includes sex workers, men who have sex with men, and young women in high-prevalence areas. Zimbabwe’s rapid regulatory action translated that global guidance into national policy faster than any other African nation.
Voices from the ground
Nyasha Sithole, of the Development Agenda for Girls and Women in Africa (DAWA) network, captured the significance plainly. “Accelerating HIV prevention for girls and young women requires an expansion of choices available,” she said. “I am excited and proud to know that my own country has approved the use of CAB-LA. This will contribute to our basket of HIV prevention tools that work for us as girls and women in Zimbabwe.”
Her framing — a “basket of tools” — points to something important. No single intervention ends an epidemic. Zimbabwe’s success so far has come from layering strategies: testing, treatment, suppression targets, and now an expanded prevention toolkit.
Hard-won progress, but real obstacles remain
Zimbabwe’s HIV response is one of the more remarkable public health turnarounds on the continent. In the late 1990s and early 2000s C.E., the country had one of the highest HIV prevalence rates in the world. Community-level treatment programs, international partnerships, and sustained political commitment drove that 84% decline in AIDS-related deaths over roughly two decades.
In 2021 C.E., Zimbabwe also launched a national strategic plan to end AIDS by 2030 C.E., aligning with global targets. UNAIDS data show the country is one of only a handful in sub-Saharan Africa to have hit all three 90-90-90 benchmarks — a genuine achievement in a region still carrying the heaviest HIV burden in the world.
The path from approval to access, however, is rarely simple. Getting newly approved drugs to the people who need them most — especially in low- and middle-income countries — involves procurement, supply chains, trained healthcare workers, and community trust. Zimbabwe’s healthcare system is under severe strain from an ongoing economic crisis, and no one at the Ministry of Health was available to comment at the time of the announcement. Those structural pressures are real and cannot be wished away.
The WHO’s commitment to support Zimbabwe in designing and implementing CAB-LA programs is a meaningful pledge, but implementation will take time, resources, and sustained coordination between government, global health bodies, and local communities. The approval is the beginning of a process, not the end of one.
A signal for the continent
Zimbabwe’s decision may carry weight beyond its own borders. Regulatory approval by a country with deep HIV experience and an established national AIDS strategy sends a signal to health authorities across Africa that CAB-LA is both safe and worth prioritizing. Médecins Sans Frontières and other access advocates have argued for years that Africa should not be last in line for life-saving HIV interventions approved elsewhere.
With roughly 25 million people living with HIV in sub-Saharan Africa — more than two-thirds of the global total — the region’s regulators moving quickly on evidence-based tools is not just symbolically important. It is a practical matter of lives.
Zimbabwe’s first-mover status in Africa on CAB-LA approval is a small but concrete piece of that larger effort.
Read more
For more on this story, see: The Guardian
For more from Good News for Humankind, see:
- Alzheimer’s risk cut in half by drug in landmark prevention trial
- U.K. cancer death rates down to their lowest level on record
- The Good News for Humankind archive on Zimbabwe
About this article
- 🤖 This article is AI-generated, based on a framework created by Peter Schulte.
- 🌍 It aims to be inspirational but clear-eyed, accurate, and evidence-based, and grounded in care for the Earth, peace and belonging for all, and human evolution.
- 💬 Leave your notes and suggestions in the comments below — I will do my best to review and implement where appropriate.
- ✉️ One verified piece of good news, one insight from Antihero Project, every weekday morning. Subscribe free.
More Good News
-
Doctors hail first breakthrough in asthma and COPD treatment in 50 years
Benralizumab, a single injection given during an asthma or COPD attack, outperformed the steroid pills that have been the only emergency option since the 1970s. In a King’s College London trial of 158 patients, those who got the shot had four times fewer treatment failures over 90 days, along with easier breathing and fewer follow-up visits. Because steroids carry real risks with repeated use — diabetes, osteoporosis, and more — a genuine alternative could change daily life for millions of people who live in fear of the next flare-up. After a half-century of stalled progress on diseases that claim 3.8…
-
Mexico launches universal healthcare for all 133 million citizens
Mexico universal healthcare is now officially a reality, with the country launching a system designed to cover all 133 million citizens through the restructured IMSS-Bienestar network. Before this reform, an estimated 50 million Mexicans had no formal health insurance, with rural and Indigenous communities bearing the heaviest burden of untreated illness and medical debt. The new system severs the long-standing tie between employment and healthcare access, providing free consultations, medicines, and hospital services regardless of income. If implemented effectively, Mexico’s move could serve as a powerful model for other middle-income nations still navigating fragmented, inequitable health systems.
-

Ghana declares its first marine protected area to rescue depleted fish stocks
Ghana’s marine protected area — the country’s first ever — marks a historic turning point for a nation gripped by a quiet fisheries crisis. Established near Cape Three Points in the Western Region, the protected zone restricts or bans fishing activity to allow severely depleted fish populations to recover. Ghana’s coastal stocks have fallen by an estimated 80 percent from historic levels, threatening food security and the livelihoods of millions of small-scale fishers. The declaration also carries regional significance, potentially inspiring neighboring Gulf of Guinea nations to establish coordinated protections of their own.