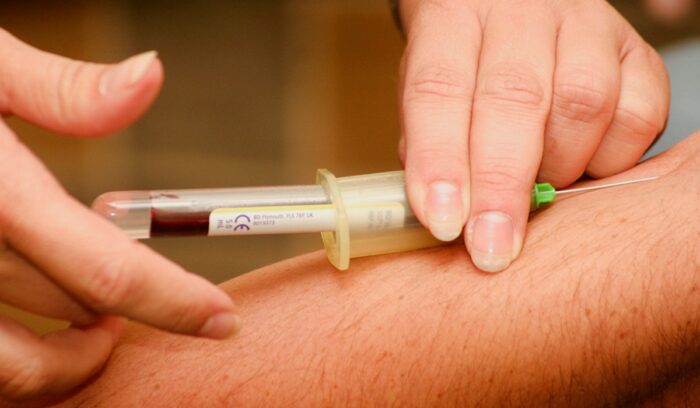
A simple blood test developed and trialed in Sweden can identify the biological signs of Alzheimer’s disease up to 15 years before a person shows any symptoms — and it performs as well as the most invasive diagnostic tools currently available. Researchers say it could open the door to routine national screening for anyone over 50, reshaping how one of the world’s most feared diseases is caught and treated.
At a glance
- Alzheimer’s blood test: The test measures levels of a protein called p-tau217 in the blood, which reflects biological changes happening in the brain during Alzheimer’s disease — and it matched the accuracy of lumbar punctures in a trial of 786 people.
- Early detection window: A University College London-led study found the test can identify early signs of the disease up to 15 years before symptoms emerge, giving patients and clinicians a meaningful head start.
- Diagnostic accuracy: Results can classify patients as likely, intermediate, or unlikely to have Alzheimer’s — potentially eliminating the need for further invasive follow-up tests for a significant portion of those tested.
What the science shows
The test, made by a company called ALZpath, is already commercially available. Its underlying science centers on p-tau217 — a protein that accumulates in the blood when Alzheimer’s-related changes are underway in the brain. The higher the levels of p-tau217, the more likely or advanced the disease.
The clinical trial was conducted by Dr. Nicholas Ashton at the University of Gothenburg and colleagues, and published in the journal JAMA Neurology. It found the test was not only comparable to lumbar punctures — which involve inserting a needle into the lower spine — but outperformed a range of other experimental tests currently in development.
Right now, confirming a build-up of Alzheimer’s-related proteins in the brain requires either that painful spinal procedure or a specialized scan available in only about one in 20 NHS memory clinics in the U.K. A blood draw changes everything about that equation.
The case for widespread screening
Prof. David Curtis, honorary professor at the UCL Genetics Institute, suggested the test could become as routine as cholesterol checks. “Everybody over 50 could be routinely screened every few years,” he said, adding that earlier diagnosis could make currently available treatments more effective — and create the conditions for even better ones to be developed.
That last point matters. Alzheimer’s treatments have historically struggled partly because patients are often diagnosed after significant brain damage has already occurred. A screening tool that catches biological changes years or even decades earlier gives researchers a far more useful window to intervene.
Dr. Sheona Scales, director of research at Alzheimer’s Research U.K., called the findings “a growing body of evidence that this particular test has huge potential to revolutionise diagnosis for people with suspected Alzheimer’s.”
Why it matters for society
The scale of the challenge makes the stakes clear. One in three people born in the U.K. today will develop dementia in their lifetime, according to the Alzheimer’s Society, which estimates around 900,000 people in the U.K. are currently living with the disease. That number is projected to rise to 1.6 million by 2040 C.E.
For individuals, an earlier diagnosis can mean earlier access to care planning, lifestyle changes, clinical trials, and whatever treatments are available. For health systems, faster and cheaper diagnosis — without the bottlenecks of specialist scans or invasive procedures — could dramatically shorten the pathway from suspicion to certainty.
Dr. Richard Oakley of the Alzheimer’s Society noted that for some patients, results could be clear enough to avoid follow-up investigations entirely — “which could speed up the diagnosis pathway significantly in future.”
What still needs work
Researchers are careful to note that more work is needed before any national screening program becomes reality. Dr. Oakley pointed out that further research across diverse communities is essential to confirm the test performs equally well across all populations who live with Alzheimer’s disease — a gap that has historically undermined the rollout of other diagnostic tools. The test identifies biological risk, not a guaranteed outcome, and the treatments that would make mass screening most meaningful are still catching up to the diagnostic science.
Read more
For more on this story, see: The Independent
For more from Good News for Humankind, see:
- Alzheimer’s risk cut in half by drug in landmark prevention trial
- Renewables now make up at least 49% of global power capacity
- The Good News for Humankind archive on global health
About this article
- 🤖 This article is AI-generated, based on a framework created by Peter Schulte.
- 🌍 It aims to be inspirational but clear-eyed, accurate, and evidence-based, and grounded in care for the Earth, peace and belonging for all, and human evolution.
- 💬 Leave your notes and suggestions in the comments below — I will do my best to review and implement where appropriate.
- ✉️ One verified piece of good news, one insight from Antihero Project, every weekday morning. Subscribe free.
More Good News
-
Doctors hail first breakthrough in asthma and COPD treatment in 50 years
Benralizumab, a single injection given during an asthma or COPD attack, outperformed the steroid pills that have been the only emergency option since the 1970s. In a King’s College London trial of 158 patients, those who got the shot had four times fewer treatment failures over 90 days, along with easier breathing and fewer follow-up visits. Because steroids carry real risks with repeated use — diabetes, osteoporosis, and more — a genuine alternative could change daily life for millions of people who live in fear of the next flare-up. After a half-century of stalled progress on diseases that claim 3.8…
-
Mexico launches universal healthcare for all 133 million citizens
Mexico universal healthcare is now officially a reality, with the country launching a system designed to cover all 133 million citizens through the restructured IMSS-Bienestar network. Before this reform, an estimated 50 million Mexicans had no formal health insurance, with rural and Indigenous communities bearing the heaviest burden of untreated illness and medical debt. The new system severs the long-standing tie between employment and healthcare access, providing free consultations, medicines, and hospital services regardless of income. If implemented effectively, Mexico’s move could serve as a powerful model for other middle-income nations still navigating fragmented, inequitable health systems.
-

Ghana declares its first marine protected area to rescue depleted fish stocks
Ghana’s marine protected area — the country’s first ever — marks a historic turning point for a nation gripped by a quiet fisheries crisis. Established near Cape Three Points in the Western Region, the protected zone restricts or bans fishing activity to allow severely depleted fish populations to recover. Ghana’s coastal stocks have fallen by an estimated 80 percent from historic levels, threatening food security and the livelihoods of millions of small-scale fishers. The declaration also carries regional significance, potentially inspiring neighboring Gulf of Guinea nations to establish coordinated protections of their own.